Click here for more information about Diabetic Retinopathy from the National Eye Institute.
Also please look at this Document for more information
If you have been diagnosed with diabetes, you may be at risk of losing sight. Your body does not utilize sugar properly and, when the sugar levels rise, damage to the retinal blood vessels may occur. The injury to the retinal vessels is known as Diabetic Retinopathy. Diabetic Retinopathy is the leading cause of blindness in working-age adults.
What are the manifestations of Diabetic Retinopathy?

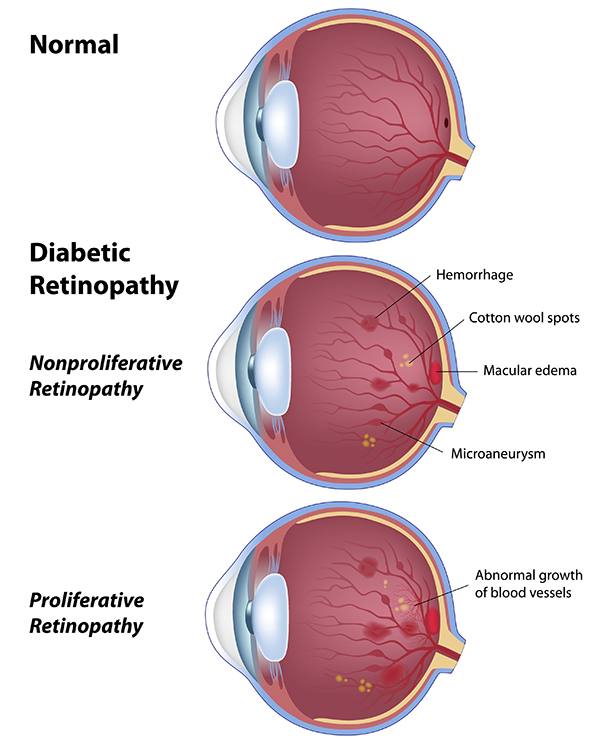
Non-proliferative retinopathy, or background diabetic retinopathy, is an early stage of diabetic retinopathy. In this stage, very small blood vessels in the retina leak blood or fluid. Many people with diabetes have non-proliferative diabetic retinopathy yet retain excellent vision. When vision is affected, it is usually the result of macular edema. Macular edema is a swelling of the macula, the region of the retina that allows us to read fine print. The swelling is caused by an accumulation of fluid that has leaked from damaged retinal blood vessels. Vision loss may be mild to severe, depending on the amount of leakage.
Proliferative diabetic retinopathy is present when abnormal new blood vessels begin growing on the optic nerve or on the surface of the retina. This occurs in response to poor circulation in the eye and the lack of oxygen delivered to the cells. These new blood vessels actually do not reestablish circulation in the retina and thus cause more harm than good. Proliferative diabetic retinopathy can cause visual loss in a few ways. Vitreous hemorrhage occurs when the fragile new vessels bleed into the center of the eye. The inside of the eye is normally filled with a clear, jelly-like substance called vitreous. Symptoms vary depending on the amount of blood that mixes with the vitreous in the eye; it can vary from a few dark floaters to near blindness of one eye. The hemorrhage may take days to months to reabsorb. If it does not clear up on its own, a surgical procedure called vitrectomy may be necessary. The visual prognosis is good if there is no damage to the macula.
Diabetic retinopathy can also lead to retinal detachments. This occurs when the new blood vessels shrink and form scar tissue that drags the retina away from its normal position. If the macula is involved, severe visual loss may occur.
Lastly, severe glaucoma may develop when the new blood vessels grow on the surface of the iris and block the normal flow of fluid leaving the eye. Pressure in the eye soars and causes damage to the optic nerve.
What are the symptoms of Diabetic Retinopathy?

Often, one may not be aware of any symptoms even when significant diabetic retinopathy is present. When macular edema occurs, vision often becomes blurry and may fluctuate.
If abnormal new blood vessels form, as in proliferative diabetic retinopathy, they may bleed and result in small specks or large floaters obscuring the vision. If a large hemorrhage occurs, vision often becomes very blurry.
How do we diagnose diabetic retinopathy?
A comprehensive eye examination by a general ophthalmologist or retina specialist is the only reliable means of detecting diabetic retinopathy. After the pupil is dilated, a device called an ophthalmoscope is used to view the retina and determine the extent of the retinopathy. If diabetic retinopathy is discovered, a fluorescein dye test and/or optical coherence tomogram (OCT) may be recommended. A fluorescein angiogram involves the injection of a dye into a vein in the arm followed by several minutes of intermittent photos with a special digital camera focused on the retina. An OCT is a non-invasive photo that creates a detailed cross-sectional image of the macula.
How do we treat diabetic retinopathy?
The best therapy is prevention. A nationwide study showed that strict control of blood sugar significantly lowered the risk of vision loss from diabetic retinopathy. Also, high blood pressure and kidney problems should be treated to minimize their effect on the retinopathy.
Laser surgery is often the first line of treatment if macular edema or proliferative retinopathy is present. For macular edema, the laser is focused on leaky areas of the retina to aid in reabsorbing the excess fluid. The primary goal of treatment is to prevent further vision loss. It is uncommon for people to recover significant vision following treatment but some do experience partial restoration. Other treatments involving medications like steroids or a novel class of medication called anti-VEGF are also often used to treat diabetic retinopathy.

For proliferative diabetic retinopathy, the laser is focused on the retina outside the macula. This pan retinal photocoagulation (PRP) treatment usually causes the new blood vessels to disappear and prevents further growth. It also decreases the risk of bleeding into the vitreous cavity.
Usually, multiple laser treatments over time are necessary to control the retinopathy. Laser surgery is not a cure for diabetic retinopathy and is not guaranteed to prevent further loss of vision.
